
Hotel Equities is a hospitality management firm that manages several hotels in Georgia. The company is a faith-based organization whose core values center around twelve statements espousing kindness, integrity, and professional conduct. Hotel Equities believes in supporting local charitable organizations and years ago became a sponsor of Lauren’s Run and CURE Childhood Cancer Annual Picnic.
This relationship grew as CURE realized the need to start a lodging program that could provide hotel stays for families who must travel long distances for treatment. Hotel Equities quickly agreed to support this endeavor and introduced CURE to the management of the Residence Inn, which is situated near Children’s Healthcare of Atlanta. This program became increasingly important during the pandemic as long-term stay facilities were forced to close.

Susan Zuppardo, Calvin Easter, and Rosa Ventura
“Because of our location, we are typically full,” said Susan Zuppardo, Regional Director of Sales for Hotel Equities. “But we always make room for a CURE family. And when a cancer patient stays for an extended period, the staff gets excited about the opportunity to give them a safe haven during a difficult time!”
While the hotel staff is committed to treating every guest like family, two little girls stand out. Raegan and Charli both suffered from the same rare brain cancer, and their families traveled to Atlanta for long-term treatment.
“These two girls and their families were amazing,” Susan said. “Even though their children were very sick, they always smiled and talked to everyone. Charli liked to have her car decorated, so we went and got special markers so we could draw on her windows.”

Raegan
Raegan and her family stayed at the Residence Inn for 12 weeks while she endured very difficult treatment. The entire staff worked hard to make the hotel a home away from home for them. Calvin, the hotel’s Chief Engineer, took ownership of being their personal shuttle service to and from treatment. There were days when he worked late, staying until he got the call to pick them up. Rosa, the property’s Executive Housekeeper, understood the anxiety of a cancer patient during COVID-19. So she always made sure everything was extra clean in their rooms. The love and care the family received at the hotel spread out even further.
“I followed their story on Facebook and talked about them to my family all the time,” Susan said. “When my sister in Connecticut heard Raegan loved unicorns, she ordered a special book for her. My mother came to visit and was heartbroken because Raegan wasn’t able to bring very many toys from home. So she went out and bought a kitchen playset for her to play with during her three-month stay.”
Both girls eventually succumbed to their disease, but the friendships built during their stays have endured.
“I’ve kept the pictures they drew me and get choked up sometimes when I look at them,”
said Susan. “They became a part of our family.” The sentiment goes both ways. Raegan’s parents, Marc and Andrea, said, “Susan and crew made the Residence Inn feel like home. What stood out was that they were genuine – no fake smiles or forced ‘How is Raegan doing?’ questions. They were genuinely concerned. They went above and beyond for us because that’s the kind of people they are. We are better people for knowing them.”
We are honored to be partners in philanthropy with such a generous company. Hotel Equities has become a very important part of how we ease the burdens of families fighting cancer.
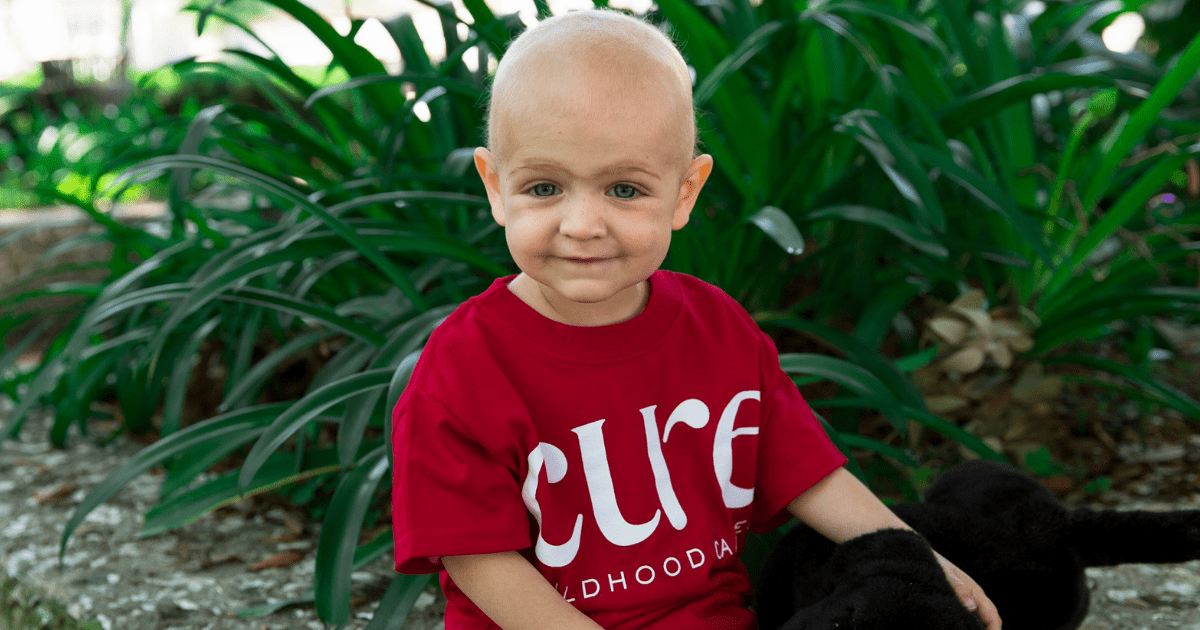
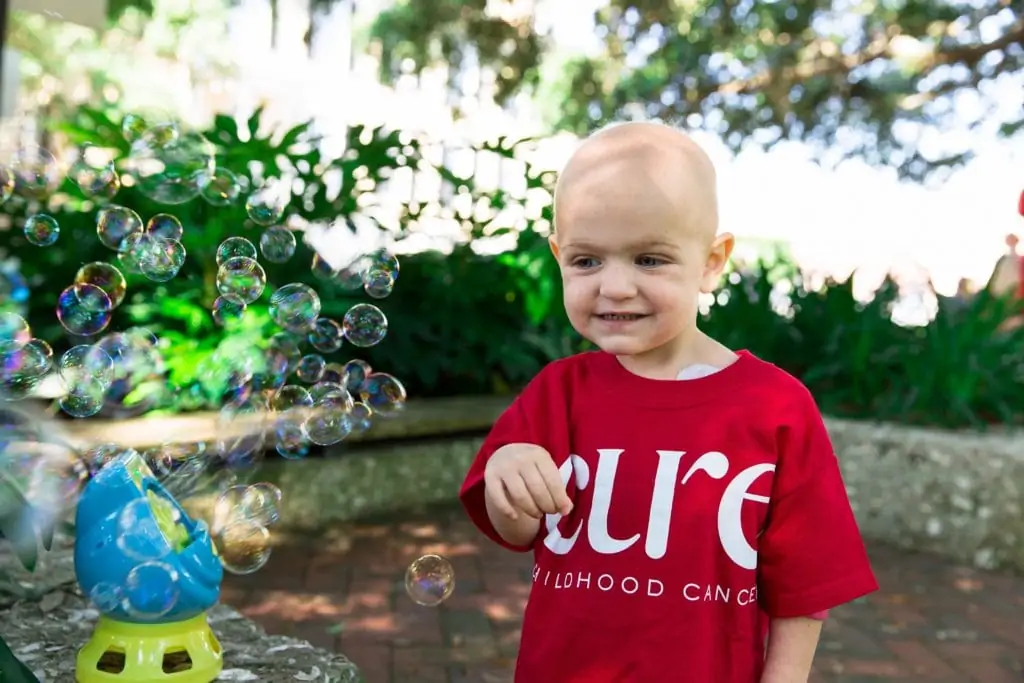 Because of her doctor’s sense of urgency, Lily’s parents suspected she might have COVID. But as the long weekend progressed and more tests were ordered, it became apparent that they were dealing with something else entirely. On Tuesday, Lily was diagnosed with acute lymphoblastic leukemia (ALL) and began her treatment.
Because of her doctor’s sense of urgency, Lily’s parents suspected she might have COVID. But as the long weekend progressed and more tests were ordered, it became apparent that they were dealing with something else entirely. On Tuesday, Lily was diagnosed with acute lymphoblastic leukemia (ALL) and began her treatment.





 The x-ray revealed a mass in Hannah’s chest near her trachea. She was admitted to the Pediatric Intensive Care Unit because the doctors worried the tumor might shift and cut off her airway. After a biopsy she was moved to the pediatric oncology floor where Hannah was diagnosed with Hodgkin’s lymphoma.
The x-ray revealed a mass in Hannah’s chest near her trachea. She was admitted to the Pediatric Intensive Care Unit because the doctors worried the tumor might shift and cut off her airway. After a biopsy she was moved to the pediatric oncology floor where Hannah was diagnosed with Hodgkin’s lymphoma.

 “Joseph was my only sibling, and we were very close,” said his sister, Rachel. “During his cancer journey, he taught me to be grateful for life’s little things. He had such a kind spirit and loved to encourage others because of the unique perspective cancer gave him.”
“Joseph was my only sibling, and we were very close,” said his sister, Rachel. “During his cancer journey, he taught me to be grateful for life’s little things. He had such a kind spirit and loved to encourage others because of the unique perspective cancer gave him.”


 Marc and his wife, Andrea, would soon learn that DIPG is a rare brain cancer for which there is no known cure. As if that wasn’t bad enough, Raegan had the worst possible genetic mutation and was given a prognosis of 6-9 months. Both Marc and Andrea work in the medical field and began scouring the internet for information and potential clinical trials.
Marc and his wife, Andrea, would soon learn that DIPG is a rare brain cancer for which there is no known cure. As if that wasn’t bad enough, Raegan had the worst possible genetic mutation and was given a prognosis of 6-9 months. Both Marc and Andrea work in the medical field and began scouring the internet for information and potential clinical trials.

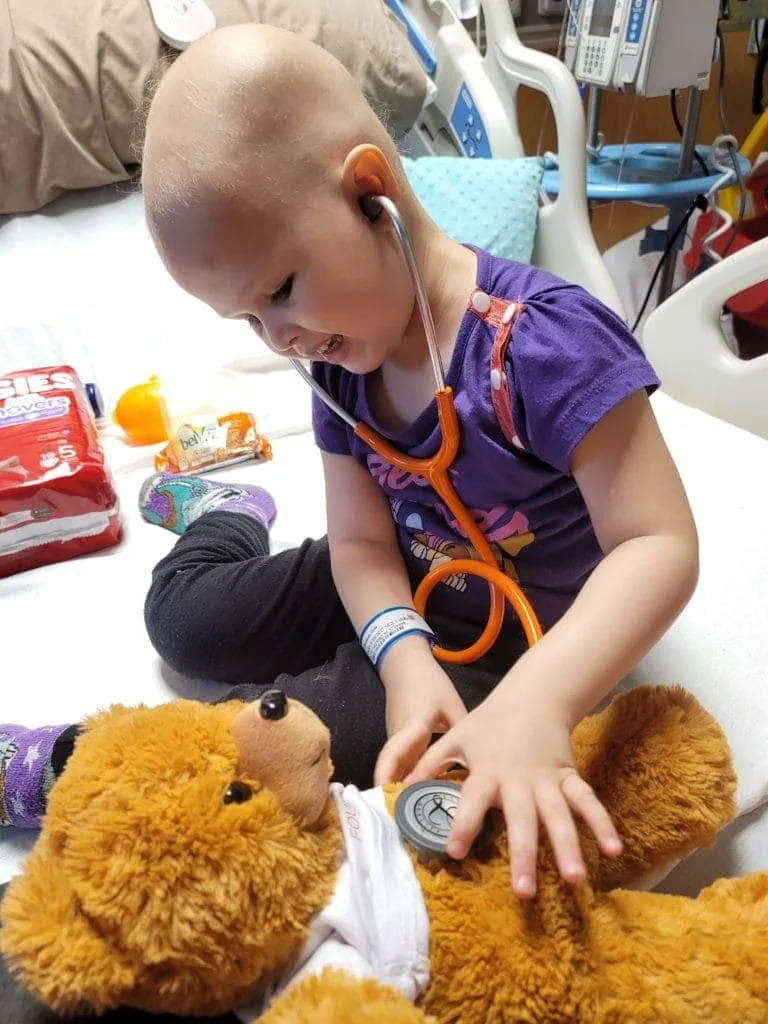 “Her whole treatment has been during the pandemic, and it adds a layer of worry,” said Courtney. “During one of her hospital stays, I was seven months pregnant. At the time, only one parent could stay with her. It’s tough to be that pregnant and alone while trying to entertain and care for a sick toddler. Being away from home so much has been difficult for her and her older brother, Arlen.”
“Her whole treatment has been during the pandemic, and it adds a layer of worry,” said Courtney. “During one of her hospital stays, I was seven months pregnant. At the time, only one parent could stay with her. It’s tough to be that pregnant and alone while trying to entertain and care for a sick toddler. Being away from home so much has been difficult for her and her older brother, Arlen.”

 “They told me Khairi had leukemia,” she said quietly. “It’s a lot to hear that your baby has cancer when you’re all by yourself. I had to leave the room so I wouldn’t break down in front of my four-year-old.”
“They told me Khairi had leukemia,” she said quietly. “It’s a lot to hear that your baby has cancer when you’re all by yourself. I had to leave the room so I wouldn’t break down in front of my four-year-old.”




