The most common causes of pediatric oncology funding gaps and the practical ways philanthropy and public-private programs help keep studies, staffing, and equipment moving.
REASON 1
A Chronic 4% Federal Funding Allocation
Pediatric cancer has long been shortchanged at the federal level. The National Cancer Institute directs a mere 5% of government research dollars toward childhood cancers – a figure that has remained stubbornly low for decades. Because children represent a small fraction of total cancer patients, funding formulas weighted by patient volume consistently deprioritize pediatric studies, regardless of the disease’s severity or the decades of potential life at stake.
KEY STAT
Less than 4% of federal cancer research funding goes to pediatric cancer, despite childhood cancer remaining the leading disease-related cause of death in children.
HOW PHILANTHROPY HELPS
Nonprofit organizations and individual donors are among the only funders who specifically target childhood cancer without competing adult-cancer priorities. Unrestricted philanthropic gifts allow researchers to pursue novel pediatric-specific trials that federal grant structures rarely support.
REASON 2
Incentive Programs for Pediatric Drug Development Are Perpetually Fragile
The Creating Hope Reauthorization Act – a Priority Review Voucher program that incentivizes pharmaceutical companies to develop drugs for rare pediatric diseases – was finally signed into law in February 2026 after years of advocacy and repeated near-expiration. The win was real, but the road to get there illustrated a systemic problem: programs like this must be reauthorized again and again, and each renewal cycle is a legislative battle that consumes enormous advocacy resources and creates investor uncertainty. Pharmaceutical companies are reluctant to commit multi-year drug development budgets to programs that may expire before a product reaches market. The hard-fought nature of each reauthorization is itself evidence of how little institutional protection exists for pediatric oncology drug development.
LEGISLATIVE FRAGILITY
The Creating Hope program has helped catalyze new therapies for rare pediatric diseases, but it required years of reauthorization fights before being signed into law in February 2026.
HOW PHILANTHROPY HELPS
Philanthropic investment in early-stage pediatric drug research helps sustain the pipeline during the inevitable gaps between legislative cycles – ensuring that promising compounds don’t die on the vine while Congress debates reauthorization.
REASON 3
Access Barriers Persist Even When Policy Wins Are Secured
The Accelerating Kids’ Access to Care Act – which streamlines out-of-state Medicaid enrollment so children can reach specialized pediatric oncology centers without dangerous delays – was signed into law in February 2026. But the access problem it addresses is far larger than Medicaid enrollment paperwork. Children on commercial insurance still face prior authorization denials that delay treatment by weeks or months. Families in rural and underserved areas still lack the financial resources to travel to the handful of specialized pediatric cancer centers in the country. And the centers themselves are chronically under-resourced relative to demand. Legislation can improve the system at the edges; it cannot replace the funding that staffs specialists, expands clinical trial availability, and brings cutting-edge care closer to where families live.
ACCESS GAP
Even with Medicaid streamlining now law, geography and insurance barriers continue to delay or deny access to specialized pediatric oncology care for thousands of families.
HOW PHILANTHROPY HELPS
Patient navigation programs, travel assistance funds, and telehealth infrastructure – often funded entirely by philanthropy – bridge the access gaps that legislation improves but cannot fully close.
REASON 4
The NIH’s Proposed 15% Indirect Cost Cap
A proposed NIH policy to cap university indirect cost reimbursements at 15% threatens to remove up to $4 billion from the broader research ecosystem. Indirect costs (covering lab maintenance, compliance staff, data infrastructure, and institutional overhead) are what make sustained research operations possible. When those reimbursements are cut, universities face a stark choice: absorb the loss, reduce research activity, or exit NIH-funded programs entirely. Pediatric oncology studies, which are already expensive and slow to enroll due to small patient populations, are disproportionately vulnerable.
FUNDING THREAT
The proposed NIH indirect cost cap could remove $4 billion from research budgets, threatening to halt ongoing pediatric cancer studies mid-stream.
HOW PHILANTHROPY HELPS
Direct philanthropic grants to research institutions can help offset indirect cost shortfalls, allowing critical studies to continue even when federal reimbursement structures tighten.
REASON 5
Clinical Trials Halting Mid-Study
When funding is withdrawn or delayed, clinical trials don’t simply pause; they often collapse entirely. Trial infrastructure requires continuous investment: staff salaries, lab reagents, patient monitoring, data management, and regulatory compliance. A funding gap of even a few months can force principal investigators to discharge enrolled patients, discard years of accumulated data, and watch the trial’s scientific validity evaporate. The children who had enrolled, and their families, are left without the experimental options they were counting on.
REAL-WORLD CONSEQUENCE
Funding gaps don’t pause clinical trials; they end them. Children enrolled in active studies may lose access to investigational treatments overnight.
HOW PHILANTHROPY HELPS
Bridge grants from philanthropic sources are uniquely positioned to sustain trials through funding gaps, preventing data loss and protecting the children already enrolled.
REASON 6
Staffing Shortages Driven by Budget Constraints
Pediatric oncology research depends on highly specialized teams: pediatric oncologists, research nurses, data coordinators, biostatisticians, and laboratory scientists. When research budgets contract, these positions are the first to be cut, and the hardest to rebuild. Unlike equipment, experienced researchers don’t sit idle waiting for funding to return. They move to better-funded fields or institutions, taking years of expertise, patient relationships, and institutional knowledge with them. Rebuilding a dismantled research team can take a decade.
STAFFING REALITY
Experienced pediatric oncology researchers who leave during funding gaps rarely return, representing an irreversible loss of institutional knowledge.
HOW PHILANTHROPY HELPS
Endowed research positions and fellowship programs funded by philanthropic donors provide job stability that attracts and retains the specialized talent pediatric oncology research demands.
REASON 7
Equipment and Laboratory Infrastructure Left Unfunded
Cutting-edge pediatric cancer research requires cutting-edge tools: genomic sequencing platforms, advanced imaging systems, biorepository storage, and precision diagnostics equipment. Federal grants typically fund personnel and direct study costs, but equipment acquisition and maintenance often fall into funding gaps. Without reliable access to modern laboratory infrastructure, researchers are forced to outsource testing, slow down timelines, or forgo studies that require technology their institution cannot afford.
INFRASTRUCTURE GAP
Laboratory equipment gaps force researchers to outsource or abandon studies—adding cost and delay to research that is already underfunded.
HOW PHILANTHROPY HELPS
Capital campaigns and equipment-specific grants from foundations and major donors can provide the durable infrastructure that neither federal grants nor institutional budgets reliably cover.
REASON 8
Early-Stage Study Financing Is Nearly Impossible to Secure
Federal funding bodies like NIH typically require preliminary data before awarding grants—but generating preliminary data requires funding. This “chicken-and-egg” problem is particularly acute in pediatric oncology, where rare cancer subtypes mean small sample sizes, and small sample sizes make it harder to generate the statistical power that reviewers demand. Promising hypotheses die in the gap between an idea and a fundable proposal, never reaching the clinical stage where they might help patients.
FUNDING PARADOX
Most federal cancer grants require preliminary data to be competitive—but collecting that data requires funding that rarely exists for early-stage pediatric studies.
HOW PHILANTHROPY HELPS
Seed grants and pilot study funding from philanthropic sources are the primary—and often only—mechanism for giving early-stage pediatric cancer research the runway it needs to become competitive for federal support.
REASON 9
The Limits of Private Funding as a Federal Substitute
As federal allocations shrink, private foundations have stepped up significantly. CURE Childhood Cancer, for example, has invested $45 million in research over the past decade and directs more than $5.6 million annually to the most promising studies. But even that remarkable commitment cannot fill a federal gap measured in billions. Private funding is also often restricted to specific projects or disease areas, making it difficult to sustain the broad, flexible research infrastructure that transformative discoveries require.
FUNDING REALITY
CURE Childhood Cancer invests more than $5.6 million annually in targeted pediatric research, but private funding cannot replace federal investment at scale.
HOW PHILANTHROPY HELPS
Unrestricted gifts to research foundations give scientists the flexibility to pursue the most promising leads, not just those that fit a narrow grant category. Recurring giving provides the stability that one-time gifts cannot.
REASON 10
Public-Private Partnership Programs Remain Underdeveloped
Perhaps the most systemic gap in childhood cancer research funding is structural: there are too few durable, well-funded public-private partnerships designed specifically for pediatric oncology. While adult cancers benefit from robust industry investment driven by large patient markets, the economics of pediatric cancer drug development rarely attract commercial interest without incentive structures like the Creating Hope Act. Filling this gap requires intentional policy design, sustained institutional commitment, and philanthropic leadership willing to catalyze partnerships that government and industry alone will not build.
SYSTEMIC GAP
Without legislative incentives and public-private partnerships, pharmaceutical companies have little economic motivation to develop drugs for rare childhood cancers.
HOW PHILANTHROPY HELPS
Forward-thinking donors and foundations can catalyze public-private partnerships by funding the convening, coordination, and early research that draws in institutional and government partners over time.
The Research Cannot Wait
Every gap in pediatric cancer research funding is a gap in a child’s chance at survival. Strategically directed philanthropic dollars can sustain clinical trials, retain specialized researchers, fund the equipment that federal grants overlook, and seed early-stage studies that federal funders won’t touch. The children enrolled in trials today and the children who will be diagnosed tomorrow are depending on it.
Support childhood cancer research funding today by donating to CURE.


 Genetic sequencing through CURE’s Precision Medicine Program revealed crucial information: her tumor carried a gene fusion called KIAA1549: BRAF. This discovery proved to be both a challenge and an opportunity. While traditional treatments would likely be less effective because of this mutation, the discovery opened the door to targeted therapies called MEK inhibitors that could block the activity of proteins that cause tumor growth.
Genetic sequencing through CURE’s Precision Medicine Program revealed crucial information: her tumor carried a gene fusion called KIAA1549: BRAF. This discovery proved to be both a challenge and an opportunity. While traditional treatments would likely be less effective because of this mutation, the discovery opened the door to targeted therapies called MEK inhibitors that could block the activity of proteins that cause tumor growth.


 Ally received her first dose of chemotherapy within 16 hours of diagnosis. Over the two years of treatment that followed, Ally struggled with almost every possible side effect. She suffered three life-threatening infections, temporarily lost the ability to walk, and struggled to rebuild her immune system after every round of chemo.
Ally received her first dose of chemotherapy within 16 hours of diagnosis. Over the two years of treatment that followed, Ally struggled with almost every possible side effect. She suffered three life-threatening infections, temporarily lost the ability to walk, and struggled to rebuild her immune system after every round of chemo.


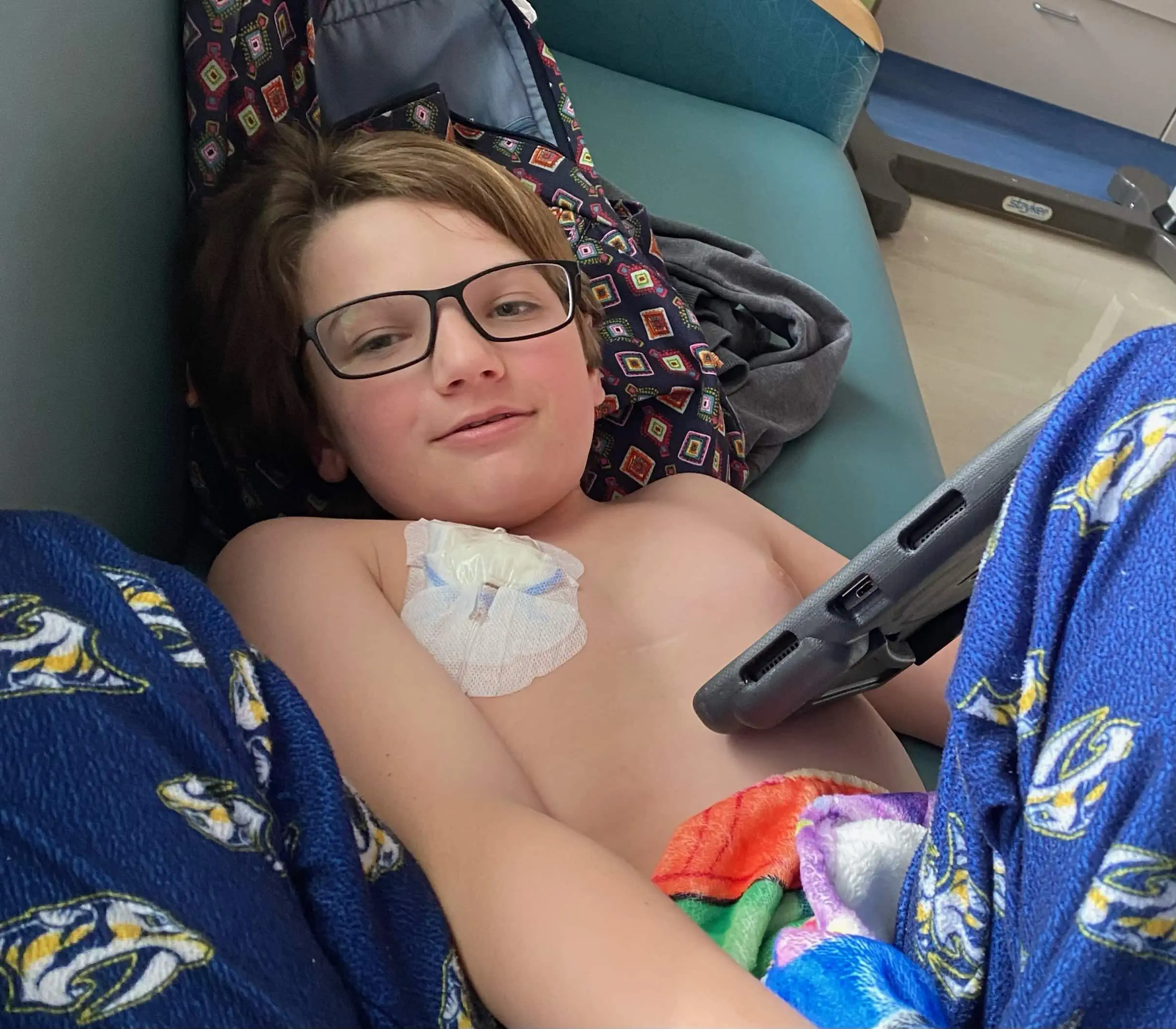 Easton had surgery to remove as much of the tumor as possible, followed by eight weeks of proton radiation in Jacksonville, Florida. His family was thrilled when a follow-up scan showed no presence of the tumor.
Easton had surgery to remove as much of the tumor as possible, followed by eight weeks of proton radiation in Jacksonville, Florida. His family was thrilled when a follow-up scan showed no presence of the tumor.